Bacterial skin infections are among the most common infections seen in India. While many are mild and readily treated, others can quickly become serious—even life-threatening. Let’s explore what causes bacterial skin infections, how they present, how they are treated, and, most importantly, how they can be prevented.
What Are Bacterial Skin Infections?
Bacterial skin infections—also called Skin and Soft Tissue Infections (SSTIs)—occur when bacteria invade the skin or the soft tissues beneath it. These range from superficial infections like impetigo and folliculitis, to deep, potentially severe infections such as cellulitis, abscesses, and necrotizing soft-tissue infection.
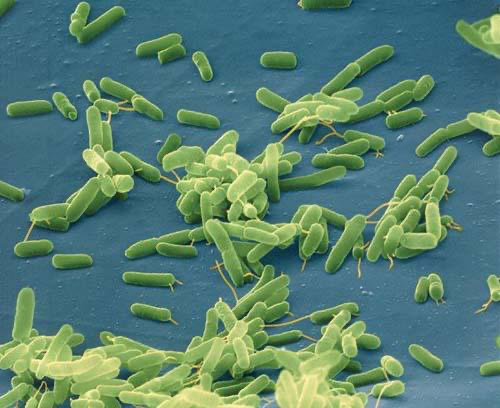
The two most common bacterial culprits are Staphylococcus aureus (including methicillin-resistant S. aureus, or MRSA) and Streptococcus pyogenes (Group A Streptococcus).
How Common Are They — Epidemiology & Risk Factors.
Skin and soft tissue infections make up a significant share of microbial disease burden. The rise of community-associated MRSA has changed the epidemiology in recent decades, leading to more complicated or recurrent infections in outpatient settings.
Risk factors can include:
- Breaks in skin barrier (cuts, insect bites, wounds).
- Underlying conditions which lowers immunity (diabetes, immunosuppression, drugs).
- Poor hygiene or crowded living conditions.
- Recurrent colonization by S. aureus.
Common Types and Their Clinical Presentation.
1. Impetigo
Cause: Often S. aureus, sometimes with S. pyogenes.
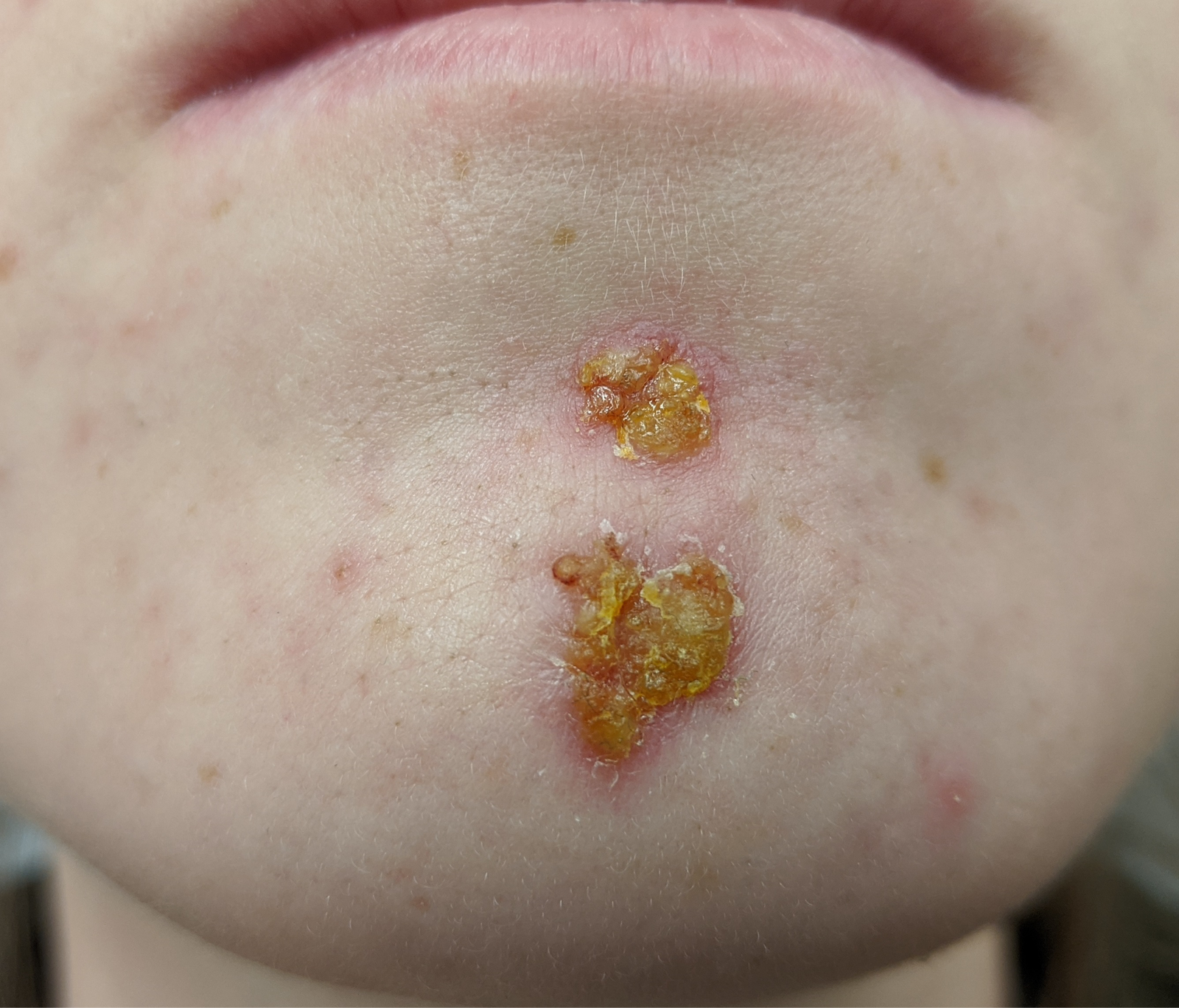
Presentation: Red sores or blisters, particularly around the nose and mouth, that ooze and form characteristic “honey-colored” crusts.
Who: Mostly children.
Complications: While rare, certain streptococcal forms can lead to post-streptococcal glomerulonephritis (injury to the kidneys).
2. Folliculitis, Furuncles, and Abscesses
Folliculitis: Inflammation of hair follicles, presenting as small pimple-like pustules.
Furuncles / Boils: Deeper infection, painful nodules.
Abscess: A localized collection of pus under the skin; often very painful and fluctuant.
Management: Warm compresses, good hygiene; abscesses often require incision and drainage, which is the primary therapy.
3. Cellulitis and Erysipelas:
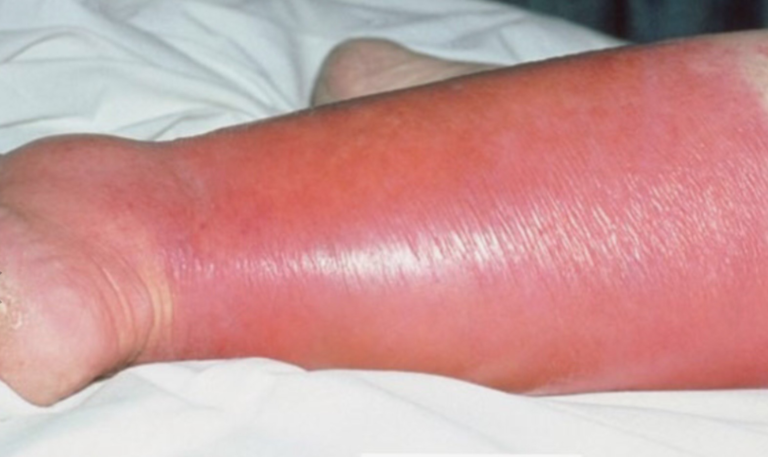
Cellulitis: A diffuse infection of deeper layer of skin and subcutaneous tissue, usually poorly demarcated, with swelling, warmth, redness, severe pain.
Erysipelas: A more superficial infection of the dermis and lymphatics, sharply demarcated, fiery red appearance.
Pathogens: Non-purulent cellulitis is typically caused by streptococci, while cellulitis associated with abscesses more often involves S. aureus.
4. Necrotizing Soft-Tissue Infections (NSTIs):
What it is: A rapidly progressive fatal infection destroying soft tissues (fascia, fat, muscle).
Symptoms: Intense pain (often out of proportion to what you see on skin), swelling, skin discoloration, systemic signs like fever, possible shock.
Urgency: This is a surgical emergency. Delays in diagnosis or surgery are often dangerous and life threatening.
5. Staphylococcal Scalded Skin Syndrome (SSSS):
Cause: Certain S. aureus strains produce exfoliative toxins A and B.
Who: Mainly infants and young children, but can affect adults with poor immunity as well..
Presentation: Blistering, widespread skin peeling that resembles a burn.
Why These Infections Are Dangerous: The Role of S. aureus:
Staphylococcus aureus is not just common — it’s also highly virulent. A recent review estimated that globally, S. aureus SSTIs contributed to over 10 lac deaths in 2019, with MRSA being responsible for many drug-resistant cases.
S. aureus uses an arsenal of virulence factors — toxins, immune-evasion proteins, and other molecules — to invade skin, evade host defense, and cause severe disease.
How Bacterial Skin Infections Are Diagnosed:
Clinical Examination: Often, the diagnosis is based on history and physical signs alone, especially for common conditions like impetigo or typical cellulitis.
Pus Cultures:
If there is pus (e.g., abscess drainage), a bacterial culture can guide targeted therapy.
The doctor collects pus safely using a sterile swab, needle, or during drainage, the sample is sent to a lab, where experts culture the sample in a petri dish and identify bacteria.
The results help guide targeted, effective antibiotic treatment.
Additional Tests: In complicated cases (suspected NSTI), imaging (CT/MRI) and lab work become critical.
Patient History: Important to consider underlying conditions, breaks in the skin, immunosuppression, drug history etc.
Treatment Strategies: Evidence-Based Approach.
1. Incision and Drainage (I&D):
For abscesses, drainage is the primary treatment. Antibiotics may be added for surrounding cellulitis, fever, large abscesses, or in patients with medical risk factors—but they never replace proper drainage.
2. Empirical Antibiotics:
Doctors often start an antibiotic that targets the most likely bacteria—Staphylococcus aureus and Streptococci.
Once the pus culture and sensitivity report is available, treatment is adjusted to a more precise, targeted antibiotic.
Topical antibiotics are only used for specific mild infections like localized impetigo.
3. Severe / Deep Infections (NSTI):
Necrotizing soft-tissue infections require urgent surgical removal of infected tissue plus broad-spectrum IV antibiotics.
These cases are medical emergencies and need hospital care.
4. Advanced or Resistant Infections:
For complicated infections—especially MRSA—doctors may use advanced antibiotics such as linezolid, daptomycin, or telavancin. These are reserved for resistant or non-responsive cases and guided by culture results.
Preventing Bacterial Skin Infections:
Prevention is central. Here are some measures to reduce risk:
Good Skin Hygiene: Wash hands frequently, keep skin clean, and promptly clean wounds or insect bites.
Barrier Protection: Cover cuts, scrapes, or abrasions with clean dressings until healed.
Avoid Sharing Personal Items: Razors, towels, or clothing can be sources of S. aureus spread, especially MRSA.
Decolonization (in recurrent cases): In people with recurrent SSTIs, decolonization strategies may be considered, under medical supervision.
Early Medical Attention: Seek prompt care when redness spreads, pain worsens, fever develops, or symptoms suggest a deeper infection.
When to Seek Medical Care — Key Warning Signs (Red Flags):
Rapidly spreading redness or swelling.
Pain out of proportion to visible skin changes.
Fever, chills, or systemic symptoms.
Skin necrosis, blistering, or signs of deep infection.
Recurrent boils or abscesses.
In immunocompromised individuals or those with diabetes.
If you or someone you know shows any of these signs, early medical evaluation is critical — particularly to rule out life-threatening conditions like necrotizing soft-tissue infection.
Conclusion:
Bacterial skin infections are common and range from mild, easily treated conditions to dangerous, rapidly progressing illnesses.
Understanding the causes, recognizing the signs early, and adopting evidence-based treatment strategies can dramatically improve patient outcomes. Equally important are preventive practices that reduce risk and curb transmission — especially in settings where drug-resistant bacteria are common.
By staying informed and vigilant—and seeking medical attention when red flags appear—you or your loved ones can navigate bacterial skin infections with confidence and safety.
References:
Clinical practice guidelines for skin & soft tissue infections. (OUP Academic)
Review of bacterial SSTI epidemiology, microbiology, pathogenesis. (PubMed)
Global clinical burden of S. aureus skin infections. (PMC)
Management of necrotizing soft tissue infections. (PubMed)
Surgical and antibiotic guidelines for SSTIs (Sartelli et al.). (BioMed Central)