Scarring is a natural part of the skin’s healing process. However, in some individuals, scars can become raised, thick, itchy, or cosmetically distressing. Two such abnormal scars are keloids and hypertrophic scars. These conditions are common in darker skin types, including Indian skin, and often require expert dermatological care for optimal management.
Keloids are abnormal scars that grow beyond the original wound boundaries due to excessive collagen production during healing. Unlike normal scars, keloids do not regress over time and may continue to enlarge slowly.
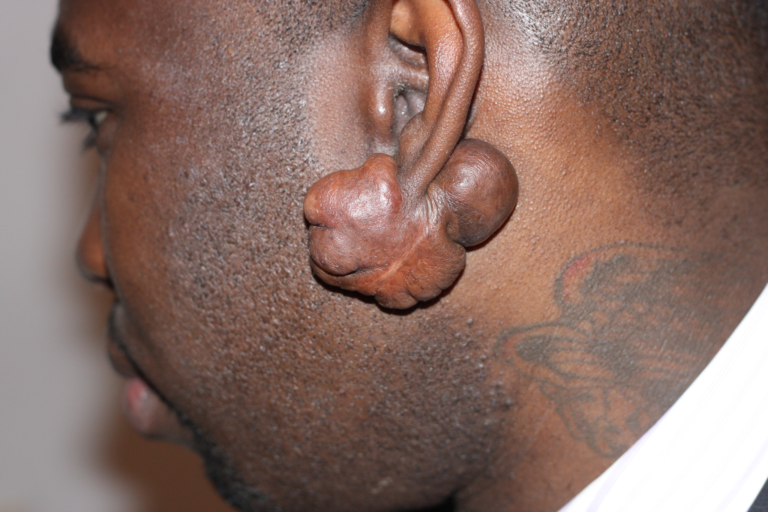
Hypertrophic scars are raised scars that remain confined to the original wound area. Unlike keloids, they may gradually flatten and improve over time.
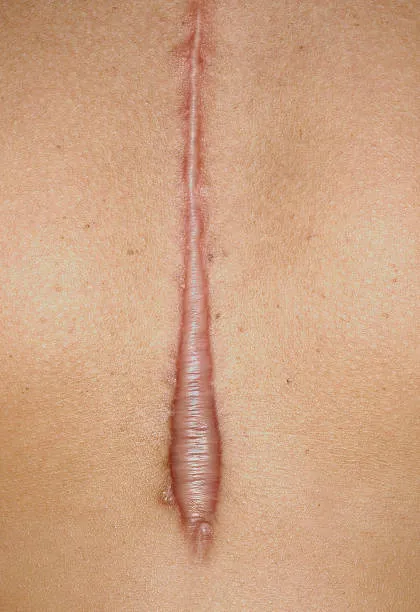
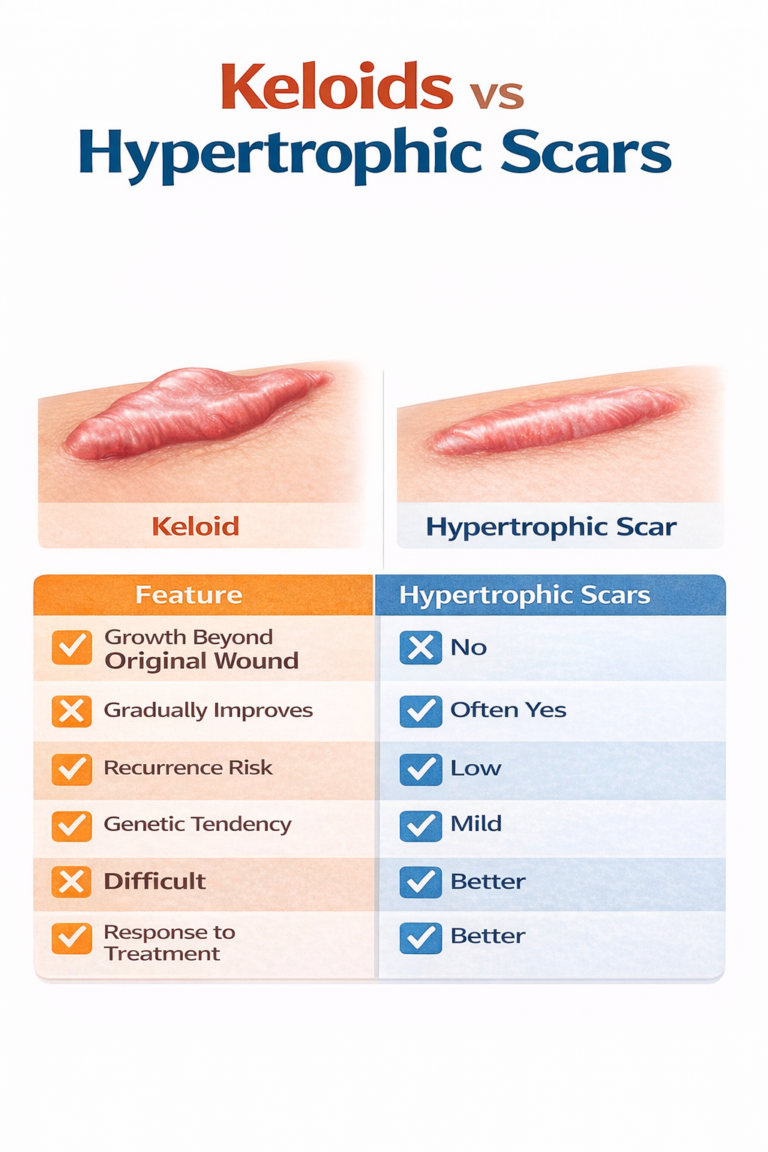
Certain individuals are more prone to abnormal scar formation.
These scars result from overactive wound healing, where fibroblasts produce excessive collagen (mainly Type III collagen). Growth factors such as TGF-β (Transforming Growth Factor-Beta) play a key role in this abnormal response.
In keloids, collagen production continues even after wound closure, leading to uncontrolled scar growth.
Management should always be guided by a qualified dermatologist, as no single treatment works for all scars.
While not always preventable, risk can be reduced.
You should consult a dermatologist if:
Early intervention significantly improves treatment success.