Urticaria and angioedema are common allergic skin conditions that can significantly affect quality of life. While they are often seen together, they involve different layers of the skin and present with distinct symptoms. Early recognition and appropriate treatment under the guidance of a dermatologist or allergy specialist are essential for effective control.
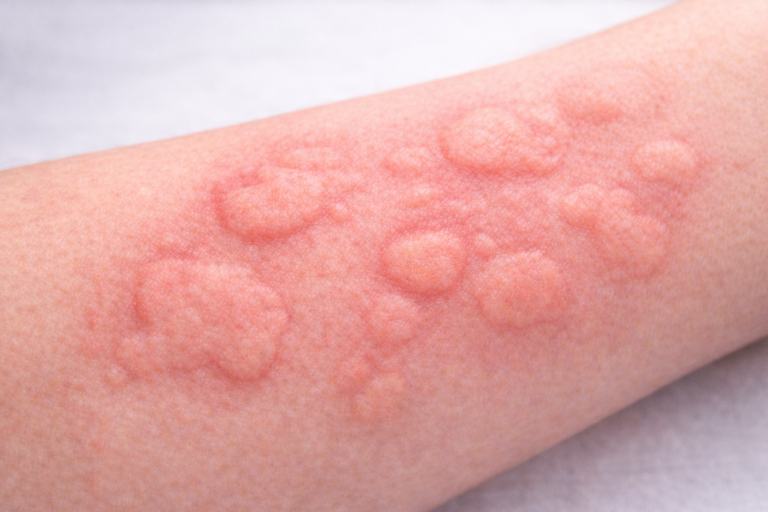
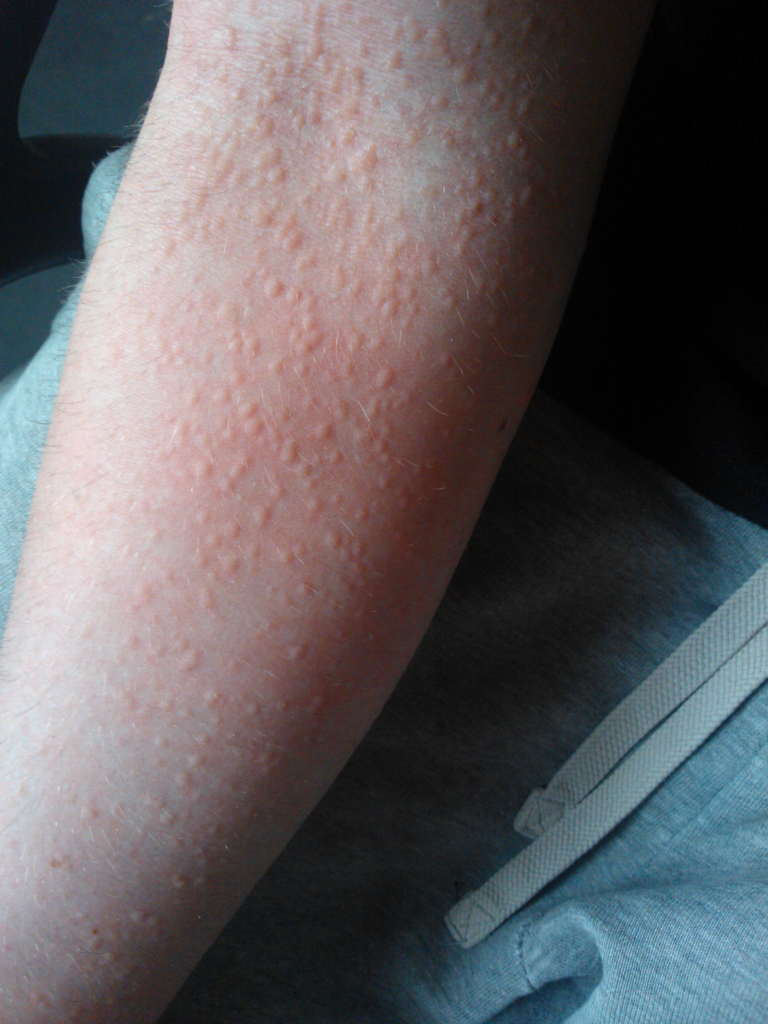
Urticaria, commonly known as hives, is a condition characterized by sudden onset of itchy, red or skin-colored raised wheals on the skin. These lesions may vary in size, shape, and location and usually resolve within 24 hours without leaving marks.
Urticaria occurs due to the release of histamine and other inflammatory mediators from mast cells in the skin.
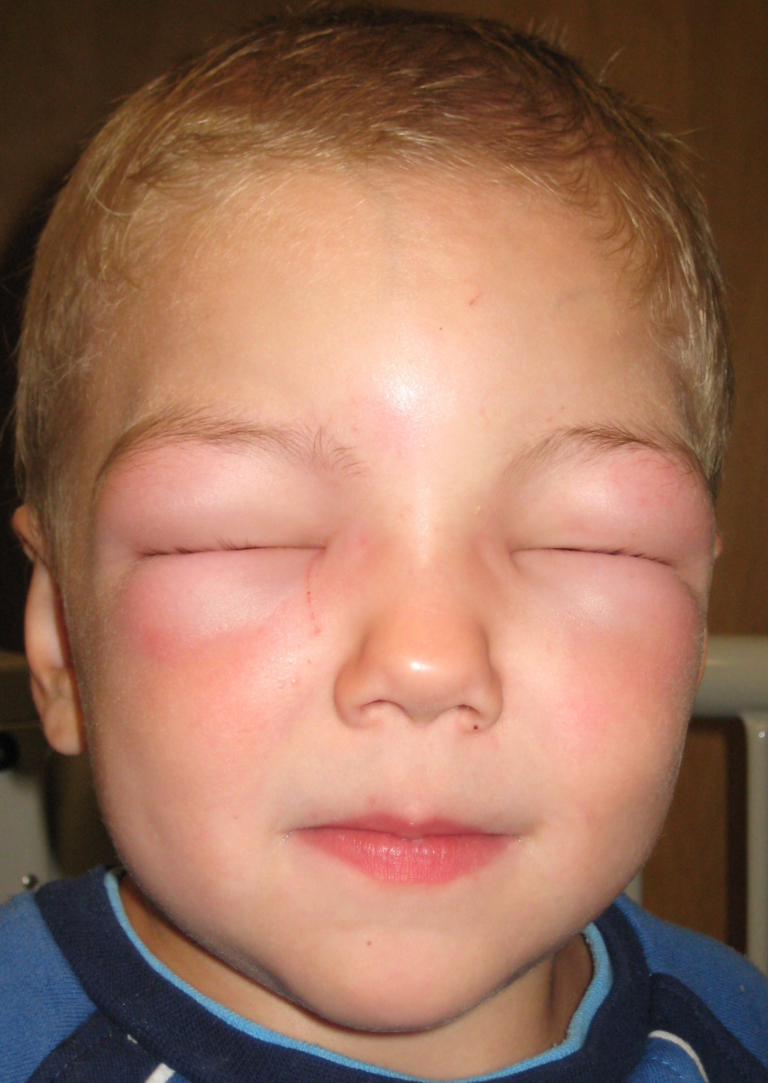
Angioedema is a deeper form of swelling that affects the lower layers of the skin and mucous membranes. It commonly involves the lips, eyelids, face, tongue, hands, feet, or genital area. Unlike urticaria, angioedema is usually painful or tight rather than itchy.
In severe cases, swelling of the tongue or throat can cause breathing difficulty and requires emergency medical attention.
Diagnosis is primarily clinical and based on history and examination. In chronic or recurrent cases, your dermatologist may recommend:

Second-generation non-sedating antihistamines are the first-line treatment for both urticaria and angioedema.
Severe angioedema involving the airway requires immediate medical care and may need injectable adrenaline.
Urticaria and angioedema are common but manageable conditions. With proper diagnosis, trigger identification, and evidence-based treatment, most patients can achieve excellent symptom control and lead a normal life.